Dieser Artikel ist noch nicht auf Deutsch vorhanden
Annex 3: Case Study of Listeria Monocytogenes in Ready-to-Eat Foods
Inhalt
Background
Listeria monocytogenes is a food-borne bacterial pathogen that can cause listeriosis, a severe disease that can result in septiceamia, meningitis and spontaneous abortion. Given the importance of this disease, the USA Healthy People 2010 goals for national health promotion and disease prevention called on federal food safety agencies to reduce food-borne listeriosis by 50 percent by the end of the year 2005. While increased government and industry attention to general aspects of L. monocytogenes control would result in some decrease in incidence, specific risk management actions were needed.This case study illustrates application of the generic RMF presented in this Guide.
Risk Management, Phase 1: Preliminary Risk Management Activities
Step 1: Identify the problem
Listeriosis typically occurs in susceptible individuals including the elderly, pregnant women and immunocompromized people (e.g. patients undergoing cancer therapy, transplant recipients and people with AIDS). Although the total number of cases in any population is relatively low (about 2,500 cases per year in the United States), listeriosis has an estimated case fatality rate of 20 to 40 percent.L. monocytogenes is widespread in the environment but the predominant food-borne disease pathway is via ready-to-eat49 foods. In addressing the L. monocytogenes problem in the United States, risk managers made an early decision to only evaluate risks associated with ready-to-eat foods because the organism is destroyed in other types of foods that are cooked or further processed before consumption.
In addition to good hygienic practice (GHP), a zero tolerance regulatory standard of no L. monocytogenes cells being detected in the food sample tested is maintained in the United States. A typical food test for L. monocytogenes is two samples at 25 grams each, which equates to a standard of less than 0.04 cfu/g. The existing regulatory standards are not achieving the level of public health protection required and better risk-based control measures are needed.
Step 2: Develop the risk profile
The concerned government agencies gathered all relevant information on L. monocytogenes in foods to inform further action. Different types of ready-to-eat foods were considered including meat products, seafood, dairy products, fruits, vegetables and delicatessen salads.Preliminary data collection activities identified many gaps in the scientific information available on L. monocytogenes in ready-to-eat foods. In particular, exposure data was deficient for a number of ready-to-eat food types and a specific survey was commissioned to fill this data gap. While most samples were found to be negative for L. monocytogenes, those that were positive typically contained less than 1.0 cfu/g, with almost all foods containing less than 100 cfu/g.
Step 3: Establish risk management goals
The primary risk management goal was to estimate relative risks associated with different types of ready-to-eat foods and develop targeted food control measures that would significantly reduce the overall incidence of food-borne listeriosis in line with USA Healthy People 2010. The relative risk ranking would identify priority food categories for risk management.A subsidiary goal was to estimate the relative risks of serious illness and death for three age-based subpopulations: i) prenatal/perinatal (16 weeks after conception to 30 days after birth); ii) the elderly (60 years of age or more); and iii) an intermediate age population.
Interventions in the ready-to-eat food chains that presented the greatest relative risks would be evaluated for their individual ability to reduce risks.
Step 4: Decide whether a risk assessment is needed
In the United States, government agencies are required to do risk assessments when making major food safety policy decisions. In this case, the risk managers decided that the most value would be gained from estimating relative risks from a wide range of ready-to-eat food categories. The decision to base control measures on estimates of relative risk was predicated by limitations in data availability.Step 5: Establish risk assessment policy
While this is a formal step in the generic RMF developed in this Guide, establishment of risk assessment policy was not conducted as a discrete exercise in this case study. However, there were a number of situations where a standardised approach to dealing with scientific data was agreed. A policy decision was made that data sets that were more recent and/or came from peer-reviewed publications would be given a higher weighting than others, and data collected outside the United States could be used if the product was imported. Exposure data would be represented as presence/absence data rather than actual numbers of L. monocytogenes in foods and this allowed all the available exposure data to be utilized in some form.For the dose-response assessment, a policy decision was made to use a non-threshold model rather than a threshold model. A non-threshold model assumes that there is a small but finite probability of illness even if only a single organism is consumed.
Step 6: Commission the risk assessment
Before commissioning, a public meeting was held to invite comment on the planned assessment and a request was made for scientific data and information to be submitted for use in the assessment. The advice and recommendations of the National Advisory Committee on Microbiological Criteria for Foods were sought on the assumptions therein and the model structure to be used.The risk assessment was carried out by the Food Safety and Inspection Service (FSIS) in the United States Department of Agriculture (USDA), the United States Department of Health and Human Services (HHS), the United States Food and Drug Administration (FDA) and the United States Centres for Disease Control and Prevention (CDC) over a period from 1999 to 2003. The risk assessment team was a multidisciplinary group of government scientists including food microbiologists, epidemiologists and mathematicians.
A total of 23 separate assessments were undertaken, which allowed an analysis of the relative risks of serious illness and death associated with a wide range of ready-to-eat food categories (http://www.foodsafety.gov/~dms/lmr2-toc.html). Primary considerations were: consumption by susceptible persons; types of contaminated foods; foods that support growth; storage time; and storage temperature.
Risk communication included presentations at scientific meetings and public meetings, the latter being held for the purpose of soliciting feedback and peer review. An initial draft risk assessment was released in 2001 to allow public comment and input from the scientific community before the assessment was finalised. This generated additional data for risk assessment and was an effective method for communicating with all stakeholders before the assessment was finalised.
Step 7: Consider the results of the risk assessment
Elements of the risk assessment are summarized in Box A3-1.The primary output of the risk assessment is shown in Figure A3-1 as estimated cases of listeriosis associated with different ready-to-eat food categories for the total United States population on a per serving basis. In the United States, delicatessen meats, frankfurters (not reheated), pâté and meat spreads pose a much greater risk (about 1 case of listeriosis per 107 servings is predicted) than hard cheeses, cultured milk products and processed cheeses, where the predicted level of illness is approximately 1 case of listeriosis per 1014 servings. The main reason for this is that the former group of foods supports the growth of L. monocytogenes to high numbers even during refrigerated storage, while the latter group does not.
The risk assessment generated risks per serving to an individual consumer and risks per annum to various populations; the latter representing total disease burden. Ready-to-eat foods ranked as very high risk, both risk per serving and per annum, included delicatessen meats and frankfurters (not reheated). This is due to high consumption, high rates of contamination and rapid growth to high numbers in stored products. Ready-to-eat foods ranked as high risk included pâté and meat spreads, smoked seafood, pasteurized and unpasteurized fluid milk, and soft unripened cheeses. Here, high relative risks are generated either from high contamination but low consumption rates or low contamination but high consumption rates e.g. pasteurized fluid milk. Ready-to-eat foods ranked as moderate risk (e.g. dry/semi-dry fermented sausages and frankfurters (reheated)) include a bactericidal step or inhibitors, so that growth to high numbers is prevented or retarded. Ready-to-eat foods ranked as low risk (e.g. preserved fish and raw seafood) have both low contamination rates and low consumption rates, and may have natural barriers to growth. Ready-to-eat foods ranked as very low risk (e.g. hard cheese) do not support growth.
The dose-response curves show that elderly and perinatal populations are more likely to contract listeriosis than the general population. The dose-response curves also suggest that the relative risk of contracting listeriosis from low dose exposures is less than previously estimated, even for susceptible populations.
| Box A3-1. Summary of elements of the risk assessment of L. monocytogenes in ready-to-eat foods Hazard characterization: Severe illness or death in three age-based populations were considered: prenatal/perinatal; the elderly; and an intermediate age population. Dose-response relationships were estimated by using contamination and growth data to predict levels of L. monocytogenes at the time of consumption for all ready-to-eat foods. These data were combined with epidemiology data to derive a dose-response model for each population group. The shape of the dose-response curve was based on mouse lethality data for L. monocytogenes but the position of the dose-response curve was fixed by anchoring the curve to annual disease statistics for the United States. Mild non-invasive listerial gastroenteritis was not considered in the risk assessment. Exposure assessment: Exposure assessments were based on estimates of the frequency of contamination of foods, the numbers of cells on ready-to-eat foods, the amount of growth before consumption, the amount of each food type consumed at a typical serving and the number of servings consumed per year. Servings per year of each ready-to-eat food category varied considerably, as did the amount of food eaten at each serving. As examples for the whole United States population, there were 8.7 *1010 servings of pasteurized milk per year at 244 g, 2.1*1010 servings of delicatessen meats at 56 g, and 2*108 servings of smoked seafood at 57 g. Initially expert opinion was used to fill a significant data gap on the length of time for which foods were stored by consumers and its effect on L. monocytogenes numbers. Later, a survey of consumer practices was commissioned by the meat industry to obtain data to allow better estimates to be made for hot dogs and delicatessen meats. Most (1,300) contaminated servings of food per person per year contained fewer than one organism per serving; 19 servings contained between 1.0 and 1,000 cfu/g; and 2.4 servings contained between 1,000 and 1,000,000. Less than one serving per person per year contained more than one million L. monocytogenes. Risk characterization: Individual food category data and the dose-response model were used to estimate the number of cases of illness per serving and per year for each food category and each population group. This allowed foods to be ranked according to two different measures of relative risk. An uncertainty analysis was performed and results were compared with existing epidemiological knowledge to validate the outputs of the risk assessment. The ability of a food to support growth of L. monocytogenes to high numbers and the opportunity for growth is a key risk factor in food-borne listeriosis. The model indicates that it is the few servings with very high levels of contamination that are responsible for most of the illnesses and deaths. |
Step 8: Rank risks
Ranking of risks associated with the 23 ready-to-eat food types was a key design element of this case study and provided the platform for the risk management options subsequently chosen. Relative risk rankings are shown in Figure A3-1.Once the risk assessment was finalised, a series of reports were released. The first report was a short executive summary of the findings. The second report was an interpretive summary, with a more detailed review of the findings. The third report was the risk assessment. A fact sheet with questions and answers was also released. By providing the information in many formats, different audiences were properly addressed.
Figure A3-1: Estimated cases of listeriosis associated with different food categories for the total United States population on a per serving basis

The box indicates the median predicted number of cases of listeriosis (log scale) and the bar indicates the lower and upper bounds (i.e. the 5th and 95th percentiles). The y-axis values are presented on a log scale. For example a log of 6 is equivalent to 1 case of listeriosis in a million servings.
DM = Delicatessen meats; FNR = Frankfurters (not reheated); P= Pâté and Meat Spreads; UM= Unpasteurized Fluid Milk; SS= Smoked Seafood; CR = Cooked Ready-To-Eat Crustaceans; HFD = High Fat and Other Dairy Products; SUC = Soft Unripened Cheese; PM = Pasteurized Fluid Milk; FSC = Fresh Soft Cheese; FR = Frankfurters (reheated); PF = Preserved Fish; RS = Raw Seafood; F = Fruits; DFS= Dry/Semi-dry Fermented Sausages; SSC = Semi-soft Cheese; SRC = Soft Ripened Cheese; V = Vegetables; DS = Delicatessen-type Salads; IC= Ice Cream and Frozen Dairy Products; PC = Processed Cheese; CD = Cultured Milk Products; HC = Hard Cheese.
Risk Management, Phase 2: Identification and selection of risk management options
The results of the risk assessment were used in different ways by the different government agencies. HHS used the risk assessment to develop a risk management action plan for L. monocytogenes (http://www.cfsan.fda.gov/ ~dms/lmr2plan.html) whereas USDA FSIS used the risk assessment primarily as a basis for new regulatory measures.United States Department of Health and Human Services (HHS)
FDA and CDC developed a risk management action plan to target the products and practices that generate the greatest risks of food-borne listeriosis. The action plan included the following objectives:- Develop and revise guidance for processors, retail outlets, food service and institutional establishments that manufacture or prepare ready-to-eat foods.
- Develop and deliver training for industry and food safety regulatory employees.
- Enhance consumer and health care provider information and education efforts.
- Review, redirect and revise enforcement and regulatory strategies including microbial product sampling.
In evaluating different risk management options, risk managers worked with risk assessors to change one or more input parameters in the risk model and measure the change in relative risk outputs. These what if scenarios included:
- Refrigerator temperature scenario, where the impact of ensuring home refrigerators do not operate above 45 °F was evaluated. Here, the predicted number of cases of listeriosis would be reduced by approximately 69 percent. At 41 °F or less, the predicted number of cases would be reduced by approximately 98 percent.
- Storage time scenario, where maximum storage time scenarios were evaluated. Limiting the storage time for delicatessen meat, for example, from a maximum 28 days to 14 days, reduces the median number of estimated cases in the elderly population by 13.6 percent. Shortening storage time to ten days results in a 32.5 percent reduction.
Additional messages to consumers and health care providers on the prevention of listeriosis were developed. These include advice on safely selecting, storing, and handling foods with special emphasis on short storage times in combination with minimising storage temperatures to as cold as necessary (and not exceeding 40 °F). Educational programmes aimed at pregnant women, older adults, and people with weakened immune systems were also updated. As examples, these population groups are advised not to eat hot dogs and luncheon meats unless they are reheated until steaming hot, soft cheese unless it is labelled as made with pasteurized milk, refrigerated smoked seafood unless it is contained in a cooked dish, and raw (unpasteurized) milk.
Regulatory risk management options include increased inspection of regulated food processing facilities that produce ready-to-eat foods ranked moderate to high risk in the risk assessment. This focuses inspection efforts on post-process contamination potential, sanitation practices, and environmental testing programmes.
Food Safety and Inspection Service, United States Department of Agriculture (FSIS, USDA)
During the development of the HHS/USDA risk assessment, FSIS initiated several regulatory actions based on current scientific knowledge with the aim of reducing food-borne listeriosis associated with meat products. When the first draft of the risk model was released in 2001, it showed that delicatessen meats (such as cooked ready-to-eat turkey or ham) presented a relatively high risk for listeriosis. As a consequence FSIS decided to focus risk management activities on delicatessen meats and initiated a further risk assessment specific to the product group. What if scenarios showed that combinations of interventions (e.g. sanitation/testing of food contact surfaces, pre- and post-packaging lethality interventions, and growth inhibitors) were much more effective than any single intervention in reducing estimated risks from deli meats (http://www.fsis.usda.gov/PDF/ Lm_Deli_Risk_Assess_Final_2003.pdf).As a consequence, FSIS amended its regulations to require that official establishments that produce certain ready-to-eat meat and poultry products put in place specific controls to prevent contamination with L. monocytogenes if those products are exposed to the environment after lethality treatments. So as to provide flexibility to industry, the regulatory rule allows establishments to incorporate one of three strategies: i) employ both a post-lethality treatment and a growth inhibitor for L. monocytogenes on ready-to-eat products; ii) employ either a post-lethality treatment or a growth inhibitor; or iii) employ sanitation measures only. These in-plant requirements are underpinned by new compliance guidelines and FSIS inspection procedures (see below).
Regulatory change was accompanied by education and outreach programmes. These risk communication activities were harmonized with those of FDA to ensure that consumer messages on listeriosis remained consistent.
Risk Management, Phase 3: Implementation
United States Department of Health and Human Services (HHS)
FDA and CDC continue to work on implementation activities, including disseminating guidance for processors. Technical assistance is provided to small and very small establishments (e.g. dairy facilities) on an ongoing basis.Consumer information and education efforts continue, including specific education packages for highly susceptible population groups and medical guidance for health care professionals. An example of a targeted education programme is that to Hispanic women of child-bearing age to only eat fresh soft cheeses made with pasteurized milk.
Regulatory risk management options that focus on increased inspection of establishments that produce high risk ready-to-eat foods have also been implemented. FDA is also working with states to eliminate the unlawful production and sale of raw milk soft cheeses.
Food Safety and Inspection Service, United States Department of Agriculture (FSIS, USDA)
A specific aspect of implementation of the new FSIS regulations is the matching of FSIS verification activities to the specific control strategy chosen by the processor. Establishments that chose sanitary measures alone have the highest frequency of inspection whereas establishments that chose both a post-lethality treatment and a growth inhibitor for L. monocytogenes on ready-to-eat products are subject to FSIS activity that only focuses on verification of post-lethality treatment effectiveness. This way, establishments are encouraged to select the most effective strategies to control for L. monocytogenes. FSIS also places increased scrutiny on operations that produce hotdogs and delicatessen meats. Compliance guidelines to control L. monocytogenes in post-lethality exposed ready-to-eat meat and poultry products were published in the United States Federal Register in May 2006 (http://www.fsis.usda.gov/oppde/rdad/FRPubs/97-013F/LM_Rule_Compliance_Guidelines_May_2006.pdf).FSIS is currently working on a risk-based L. monocytogenes verification algorithm that rewards highly-performing establishments by reducing inspection frequency.
Risk Management, Phase 4: Monitoring and review
United States Department of Health and Human Services (HHS)
The risk management action plan developed by FDA and CDC also includes the objectives of:- Enhance disease surveillance and outbreak response.
- Coordinate research activities to refine the risk assessment, enhance preventive controls, and support regulatory, enforcement, and educational activities.
To detect illness outbreaks more quickly and accurately, CDC is continuing to increase the number of laboratories capable of L. monocytogenes analysis through CDCs PulseNet laboratory network and will evaluate additional methods for rapid subtyping of pathogenic strains. A CDC comprehensive case-control study to gather additional information about food-borne listeriosis is also being undertaken.
Risk managers identified a number of future research needs to refine the existing risk assessment so as to facilitate review the risk management options chosen. These include scientific evaluation of: the effectiveness of post-packaging pasteurization; use of bacteriocins, irradiation, high pressure processing, and inhibitory compounds to eliminate or prevent the growth of L. monocytogenes; and development of improved epidemiological methods for food source attribution.
Food Safety and Inspection Service, United States Department of Agriculture (FSIS, USDA)
Establishments must share data and information relevant to their controls for L. monocytogenes with FSIS. Additionally, FSIS carries out its own random testing of ready-to-eat meat and poultry products and this is used to rank establishments for verification purposes. These data are subject to ongoing evaluation, with review of regulation if necessary. It should be noted that human health surveillance as a specific monitoring and review activity is not within the jurisdiction of USDA.Risk communication
Risk communication was incorporated at various points throughout the risk analysis as indicated in the above discussion. Different approaches were used to communicate with external stakeholders about the nature and effects of the specific food safety risks faced. These included public meetings and calls for scientific data and information before the risk assessment was commissioned, public meetings to seek feedback from interested groups (including the scientific community) and peer review an initial draft risk assessment, and complementary activities to enhance knowledge among consumers and health care providers about the prevention of listeriosis.In the case of proposed risk management options for ready-to-eat meat and poultry products, FSIS published proposals for interim regulatory requirements in the Federal Register and are continuing to engage with industry on practical aspects of their implementation.
Risk analysis offers a tool that national food safety authorities can use to make significant gains in food safety. Encompassing three major components (risk management, risk assessment and risk communication), risk analysis provides a systematic, disciplined approach for making food safety decisions. It is used to develop an estimate of the risks to human health and safety, to identify and implement appropriate measures to control the risks, and to communicate with stakeholders about the risks and measures applied. Risk analysis can support and improve the development of standards, as well as address food safety issues that result from emerging hazards or breakdowns in food control systems. It provides food safety regulators with the information and evidence they need for effective decision-making, contributing to better food safety outcomes and improvements in public health.
FAO and WHO have developed this Guide to assist food safety regulators understanding and use of risk analysis in national food safety frameworks. The primary audience is food safety officials at the national government level. The Guide provides essential background information, guidance and practical examples of ways to apply food safety risk analysis. It presents internationally agreed principles, a generic framework for application of the different components of risk analysis, and wide-ranging examples rather than prescriptive instructions on how to implement risk analysis. It complements and is aligned with other documents that have been produced or are being developed by FAO, WHO and the Codex Alimentarius Commission.
This Guide is the first part of a two-part set, all of which is available on CD-ROM. The second part comprises a number of educational elements for capacity building, which include a slide presentation for use in training, a collection of up-to-date FAO and WHO tools and training materials related to food safety risk analysis, and specific examples and case studies of risk analysis carried out at the national and international level.
Notes:
49
Products that may be consumed without any further cooking or reheating
 Nach oben
Nach oben



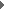 Firmen
Firmen